When word started coming from Seattle in late February about how bad this new virus COVID-19 could be for hospitals, it was imperative small community health systems like Newport Hospital and Health Services get ready.
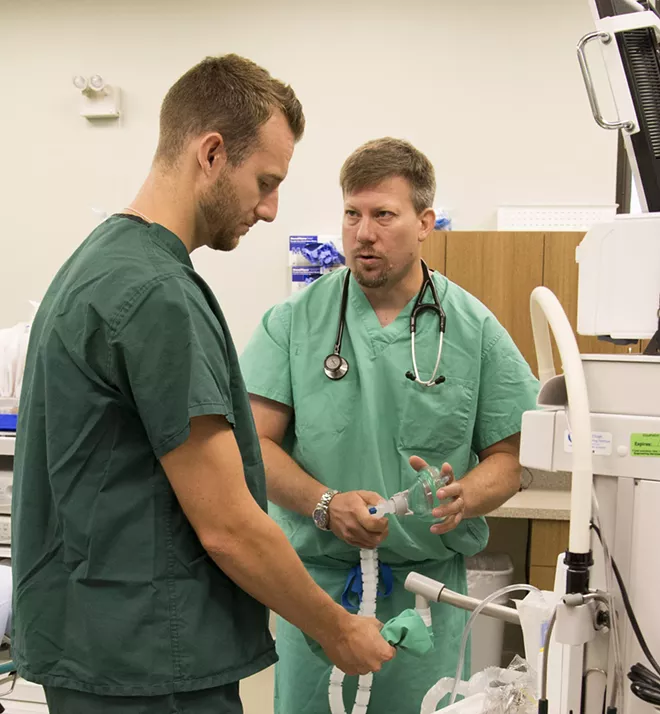
Family physician Dr. Geoff Jones knew that even during normal times, the 24-bed critical access hospital in Pend Oreille County had to provide intensive care unit-type service to patients whenever the ICUs in Spokane and Coeur d’Alene were full.
“It seemed like every month there’d be somebody here requiring ICU care and there wasn’t an ICU bed available in the region,” Jones says. “I remember one patient, for three days, twice a day, I called Kootenai [Health], Sacred Heart, Deaconess and the Valley and they didn’t have an ICU bed, so we were forced to keep that patient here.”
While doctors make do with cases like that one, if that’s how things are during normal times, Jones thought, they could be far, far worse if a viral outbreak overwhelmed the region.
Jones is also the assistant clinical dean for the University of Washington School of Medicine’s students who train in Central and Eastern Washington rural hospitals. That decadeslong partnership has connected the medical school with rural hospitals in Washington, Wyoming, Alaska, Montana and Idaho.
Students in their clinical rotations were pulled from the hospitals this spring due to concerns about conserving personal protective equipment like surgical gowns and masks. However, the close relationship with colleagues in Seattle who were the first in the country to deal with a COVID outbreak meant the small public hospital district in northeast Washington was quick to make adjustments, even outpacing some of the larger hospital systems in Spokane, Jones says.
“We were able to restrict visitors and institute strict controls into our assisted living nursing home, and we were able to start temperature screening in the clinic 10 days before Providence did in Spokane,” Jones says. “Again, that’s because of that relationship, and because we’re a small hospital system and we don’t have to go through a larger system for approval.”
Luckily, Pend Oreille and other small northeastern Washington counties largely avoided an outbreak, with some seeing only one or two confirmed cases.
But even as many small and rural counties have so far been lucky to avoid a sudden wave of COVID patients, the shift in attention is now on how to keep those counties prepared as they are among the first to reopen for business. New guidance from the state this week enabled 10 more counties to apply to move into the next phase of reopening restaurants, retail and more, but even as hospital systems feel prepared, some small rural counties are still left ineligible to reopen under the new rules.
PREPARING FOR THE WORST
When it became clear that COVID could overwhelm large health systems and leave critical access hospitals in rural areas more on their own, the small systems quickly implemented emergency planning.
For Pend Oreille County’s public hospital system, that included a quick move to convert hospital beds and create a plan to separate COVID-19 patients from general hospital patients, says Jenny Smith, public information officer for the Newport Hospital and Health System.
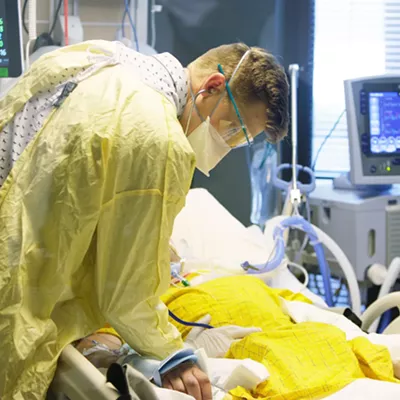
Staff quickly converted the 24 beds in the hospital’s acute care area to have negative airflow, which prevents infected droplets in the air from spreading to other parts of the hospital, Smith says.
“When all of this kicked into gear, we had the expectations that Spokane’s facilities and Coeur d’Alene’s facilities were going to be overrun and not have room in their ICU if we needed to transfer patients,” Smith says. “As a critical access hospital, we typically do transfer patients in need of ICU care to Spokane, so we had to figure out a way around this.”
Part of that meant securing ventilators for potential ICU patients. The district secured two ventilators for in-hospital care.
The community also came out in a major way, responding to the district’s request for donated personal protective equipment, giving the foundation more than $18,000 worth of face masks and surgical masks, Smith says.
Another piece that happened to work out for the district was that its long-term care facility was recently upgraded and last year, those long-term patients were moved into a new advanced care facility.
“So we had this big empty long-term care facility. Our amazing team quickly converted that into a hospital area,” Smith says. “What we had intended to do was use that for non-COVID patients we wanted to keep separate from the COVID patients.”
In the end, with only two confirmed cases in the county so far, the district didn’t have to use the separate facility, and things are starting to reopen and return to normal in a slow manner, she says.
“I would give hats off to the people who did quarantine, the people who did stay home and kind of sheltered in place, the people who are wearing masks,” Smith says. “We’ve been very fortunate.”
WAITING TO REOPEN
The virus has spread slowly in many of northeastern Washington’s counties, indicating distancing measures worked to prevent an outbreak, and allowing them to be among the first to reopen many businesses in recent weeks.
As mentioned, Pend Oreille County has had only two confirmed cases of COVID-19, in a county of about 13,600 people. Neighboring Stevens County (population: about 45,725) has had 10 confirmed cases, and Ferry County (population: about 7,650) has had one confirmed case, according to Northeast Tri County Health District numbers.
All three counties were in the first group allowed to move to phase 2 of the state’s reopening plan, returning to limited in-restaurant dining options, opening hair salons with strict guidance, and allowing retail to return.
New guidance issued by Gov. Jay Inslee on Tuesday, May 19, enabled counties that had less than 10 new confirmed cases per 100,000 people over 14 days of complete data to apply to move into phase 2 of the state’s reopening plan.
For many, that was welcome news. Leaders in Spokane County, which is home to nearly 523,000 people, cheered the fact they’d be able to apply to move to the next phase, since the county had just 34 new cases over the time period from May 5-18.
But Ferry County’s neighbor, Okanogan County, still does not qualify to move to reopen under that guidance. Initially, the county was told it would have to go 21 days without a single case. Under the new guidance, Okanogan needs to go 14 days without more than four new cases.
As of May 21, the county had seen a total of 44 cases among its 42,730 residents since tracking began two months ago, but there were too many cases over the two-week period of data observed by the state to allow the county to apply for phase 2 approval, according to the state Department of Health.
“We all want to open again, but safely. Those are two laudable and appropriate goals, but we don’t necessarily agree on the best way to get there,” says Dr. John McCarthy, who is serving as a public health liaison for Okanogan County during the pandemic. “We didn’t qualify for the variance that some other counties did, and that’s very frustrating for the economic drivers.”
Initially, public health officials in Okanogan were largely focused on preparing the different hospitals throughout the valley for an outbreak, and it was decided the North Valley Hospital wouldn’t take COVID patients because it shares space with an assisted living facility, McCarthy says.
“They’re losing their business, they’re angry, frustrated, that’s their livelihood, we totally get that. And yet, we have to comply.”
Once plans were in place for obtaining personal protective equipment, test kits, and screening staff for fevers and symptoms, the next focus became public education and contact tracing. With 11 of the 44 cases so far occurring on the Colville Reservation, Okanogan County Public Health has worked closely with the Confederated Tribes of the Colville Reservation to trace contacts with confirmed cases, says Lauri Jones, community health director for the Okanogan health district.
While the preparation side of public health has gone fairly well, Jones says at this point there’s palpable frustration among business owners in the community. The health district met with owners last week to talk about what the next phase would look like, and many voiced their concerns that they’re still not allowed to open their small businesses.
“They’re frustrated when it’s a one-person salon and yet all these people are going into Walmart,” Lauri Jones says. “They’re losing their business, they’re angry, frustrated, that’s their livelihood, we totally get that. And yet, we have to comply.”
The district has faced threatening and angry comments on social media during efforts to share public health information throughout the pandemic. For the most part, Jones says she thinks people have been positive and understanding, but sometimes the negative voices are the loudest. Some are critical of guidance to wear masks in public, while others question whether the virus is really a big deal.
In combating misinformation, one of the main messages she continues to share is that the virus really doesn’t discriminate. It can, in fact, affect healthy, young people: One of their hospitalized patients was someone with no underlying health conditions in their 30s, who wound up in the hospital for nine days, she says. At the same time, Jones says she’s reminding people that the numbers have thankfully stayed fairly low due to the social distancing and shutdown measures in place.
“Because we have been taking these precautions, we believe that we’re ahead because of that and because they were implemented early,” she says. “As it becomes more tangible here, I truly believe people are wanting to do the right thing for the majority. It’s the handful that doesn’t.”