By Joy Borkholder / Crosscut.com / July 6, 2022
At the beginning of the pandemic, administrators at tiny Summit Pacific Medical Center in Elma, Grays Harbor County, thought they had a good plan to manage COVID-19 patients. They would send patients about 30 minutes east to Providence St. Peter Hospital in Olympia in exchange for taking non-COVID-19 admissions.
Such transfers are routine for Summit Pacific. Its staff frequently stabilizes patients before transporting them to a higher level of care at another hospital.
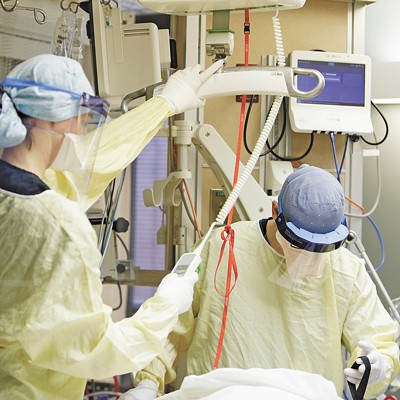
But the plan didn't work. As the first wave of infections maxed out Providence St. Peter around May 2020, Summit Pacific redeployed staff to its emergency department. At one point 80% of patients needed COVID-19 care and three people were on ventilators. The hospital had to start admitting them.
It sometimes had 20 emergency department patients, forcing it to cut inpatient beds from 10 to five, Summit Pacific officials said. Staff from other units and high-level administrators with medical licenses stepped in to care for patients. They converted conference rooms to clinic space and, later, vaccine stations.
Summit Pacific CEO Josh Martin said the hospital gratefully received $4.7 million in CARES Act Provider Relief Funds in 2020. Together with a $4.6 million Paycheck Protection Program loan, those dollars "saved" the hospital, he said, allowing it to cover payroll and keep everyone on staff.
Many small, rural medical centers classified as "critical access hospitals" struggled with financial sustainability long before the pandemic. In some cases, federal relief money offered the only hope of continuing care and may have masked financial losses amid increased costs and volatile income. Despite millions of dollars in federal support, a recent report estimated 14 Washington hospitals remain at risk of closing in the next six years.
In Washington state, many of these rural hospitals are also public hospitals that undergo routine audits published by the state. But private systems can be far less transparent with how they distribute federal dollars across complex organizational structures, making it hard to account for how much money gets to the local level.
And, as COVID-19 lingers, hospitals continue to struggle to hire enough staff, keep up with inflated operational costs and care for patients who show up sicker after putting off medical appointments the past two-plus years.
"COVID's still here," Martin said, "and we're still in crisis in many ways."
RURAL CARE AT RISK
The future of some of Washington's rural hospitals remains precarious, according to Jacqueline Barton-True, vice president of advocacy and rural health at the Washington State Hospital Association. She said the pandemic has posed "multiple, unfolding challenges at once," and it's not over.
At the most basic level, these hospitals provide access to emergency departments for rural Washingtonians, who otherwise might have to travel more than 30 minutes to get life-saving care. But they also tend to treat older, sicker patients and higher shares of Medicaid or Medicare patients, who draw lower reimbursements that may not cover the full costs of care. Some also provide expensive hospice and ambulance services over large geographic areas.
"Rural health care is just a challenge to make work financially, fundamentally," Barton-True said.
While these facilities offer important services, she said, they don't have the steady volume of patients that the U.S. health care payment system relies on. Federal Provider Relief Funds proved "vital" to keeping many of them open these past two years.
Cascade Medical Center in Leavenworth is also a small, critical access hospital with a regional plan in place to send COVID-19 admissions to the much larger Central Washington Hospital in Wenatchee. In this case, the plan worked and Cascade Medical had not admitted any COVID-19 patients through May of this year.
But CEO Diane Blake said Cascade Medical has still needed state and federal relief. She described a $2.2 million Paycheck Protection Program loan as "really essential for us because it was a way to keep going." It helped avoid staff furloughs in the earliest days of the pandemic, despite closing some specialty services and moving other care to telehealth.
With the $4.3 million Cascade Medical received in Provider Relief Funds, Blake said the hospital bought more beds and defibrillators, improved the HVAC system for infection control, replaced the lab refrigerator for vaccine storage and sponsored vaccine clinics.
"The federal dollars helped us stay open and prepare a little bit for the future," she said. "We were able to replace some items that made sense from the pandemic perspective, but will also mean we don't have to replace that two years from now."
However, Blake worries that the much-needed federal relief might be masking a "crisis in the making." Capped reimbursements, staffing shortages and rising costs for care continue to squeeze rural health facilities.
"We still have a problem in rural health care of the payments," she said. "And the way payment methodologies are set up ... they don't necessarily sustain care."
Like Summit Pacific, Cascade Medical is a public entity — Chelan County Public Hospital District No. 1 — with open commissioner meetings and financial reports. Public hospitals must comply with transparency rules that most private providers do not, leaving gaps in comparing how facilities have invested their relief money.
And similar to many small, rural entities receiving significant federal funding for the first time, Blake said, Cascade Medical is also preparing for its first "single audit" — a challenging effort for its shorthanded finance department.
DISPARITIES IN TRANSPARENCY
More than 20 miles down Highway 2 at Central Washington Hospital, nurse Paul Fuller said he has watched fellow health care workers leave "in droves'' amid intense schedules, heavy patient loads and mounting burnout. Some took attractive travel nurse contracts that offered significantly higher pay. Others felt stretched thin by staff turnover or left in the dark about how hospital administrators planned to address the crisis.
"Hospitals as a whole need more transparency, across the board," he said. "Because it is a teamwork job. ... Staff should be able to know what's going on."
If the hospital would have told staff where the pandemic relief money was going, any restrictions on it, and why there wasn't enough to give them hazard pay or retention bonuses early on, Fuller said, it would have made him feel a lot more respected. He said he thinks it also would have prevented some of his co-workers from leaving.
The reporting requirements on federal relief, such as Provider Relief Funds, may appear robust, despite delays on plans for post-payment review or audits. The reporting can be time-consuming and detailed, according to administrators such as Blake. But private hospitals are not required to share any of that with their employees or the broader community.
Central Washington Hospital is owned by a private nonprofit, Confluence Health. A spokesperson declined to confirm the amounts the hospital received in federal pandemic relief, how it used the money or details of its current financial stability. Confluence's audited financial statements are not public record, and its IRS tax filing (Form 990) has not been posted for 2020.
In its 2021 Community Report, Confluence writes that CARES Act money helped it "maintain a positive operating margin." According to federal data, Confluence's two hospitals and perhaps other related entities received $34.7 million in Provider Relief Funds.
Multistate systems PeaceHealth and Providence St. Joseph Health both agreed to share some information with Crosscut about the pandemic relief attributed specifically to some of their hospitals in Washington state. Otherwise, federal awards to large hospital systems often obscure what dollars make it down to local hospitals.
For example, Crosscut estimated that Providence St. Mary Medical Center in Walla Walla received $5.5 million in Provider Relief Funds listed under two iterations of the name Providence Health & Services — Washington, in Walla Walla. But Providence's spokesperson confirmed it received $15.6 million.
In response to these reporting gaps, health care unions and other advocates pushed for hospitals to report not just to the government, but also to their communities about their usage of federal relief dollars and other activities during the pandemic.
"More transparency is always better," said Ruth Schubert, a spokesperson for the Washington State Nurses Association, which represents staff at Central Washington Hospital.
In Washington state, a 2021 law (House Bill 1272) will soon require hospitals to report to the state Department of Health more detail on expenses and revenues, emergency grants and loans (such as during the current pandemic), patient demographics, charity care and more.
Similarly, Community Catalyst, a national nonprofit focused on health equity, sent a letter to U.S. Secretary of Health and Human Services Xavier Becerra in August, requesting greater accountability and transparency of federal pandemic relief funds.
And, it argued, grants to health care providers should be conditioned on those providers taking "concrete steps to address health inequities." Those steps could include suspending medical debt collection activities during and for at least one year after the end of the public health emergency.
Mark Rukavina, program director at Community Catalyst, said no new restrictions have yet been imposed, but his organization continues to advocate for tighter rules on future relief dollars.
"We'd like to see clear conditions put on that funding," he said, "so that it's a benefit both to those hospitals or health care providers, as well as to the patients served by those providers."
"It's a lot of communities, a lot of hospitals trying to hang on, doing their best in responding to events as they can."
tweet this
ONGOING CHALLENGES
Critics of the early rounds of Provider Relief Funds argue that the program disadvantaged rural hospitals or small providers while giving money to systems with large cash reserves that could weather the tumult without help. Some of those systems bought up other providers, as places like Cascade Medical and Summit Pacific had to suspend specialty care. System administrators disputed those alleged disparities, contending that all hospitals faced historic challenges.
Barton-True of the Washington State Hospital Association said rural hospital leaders continue to voice uncertainty about when or if they will get back to pre-pandemic operations.
"It's a lot of communities, a lot of hospitals trying to hang on, doing their best in responding to events as they can," she said. "But looking forward right now is really challenging."
Industry reports show inflation has hit hospitals hard in pharmaceuticals and other supplies, with an average overall expense increase of 20% from 2019 to 2021. Hospitals cannot just raise prices in response to inflation, as a private business might. They negotiate payment rates with insurance companies and take what the government pays in Medicare and Medicaid rates.
While the hospitals are absorbing costs right now, eventually patients will, in the form of higher premiums and out-of-pocket expenses.
Summit Pacific in Elma and other rural hospitals have closed some specialty services, forcing patients to delay care or travel farther for appointments. Officials at Summit Pacific and Cascade Medical both described delayed care or screenings that have resulted in seeing more patients with more severe needs.
The Washington State Nurses Association has also advocated for hospitals to pay more to hire and retain current staff, as a way to save money on expensive travel nurses. Schubert said it feels as though some rural hospitals are recognizing this in recent negotiations with the union and started offering some retention bonuses and wage increases.
While Summit Pacific has paid employees $320,000 in "retention incentives" over the past two years, CEO Martin said rural hospitals "cannot win" on wages or bonuses relative to larger, big-city hospitals, nor the temporary staffing agencies.
The Washington State Hospital Association is still lobbying for federal financial assistance, such as more Provider Relief Funds to cover the months including the delta and omicron surges. But those funds appear to be dried up, while the hospitals and communities still face COVID-19, sicker patients and high inflation.
"The challenge is that we're really struggling to convince people that this is still happening for us, that hospitals are still very much in the midst of COVID and will be for some time," Barton-True said. "And we're probably going to be the last to be able to be done with COVID, if we ever are." ♦
Visit crosscut.com/donate to support nonprofit, freely distributed, local journalism.