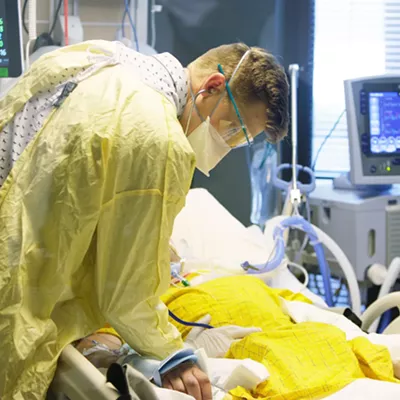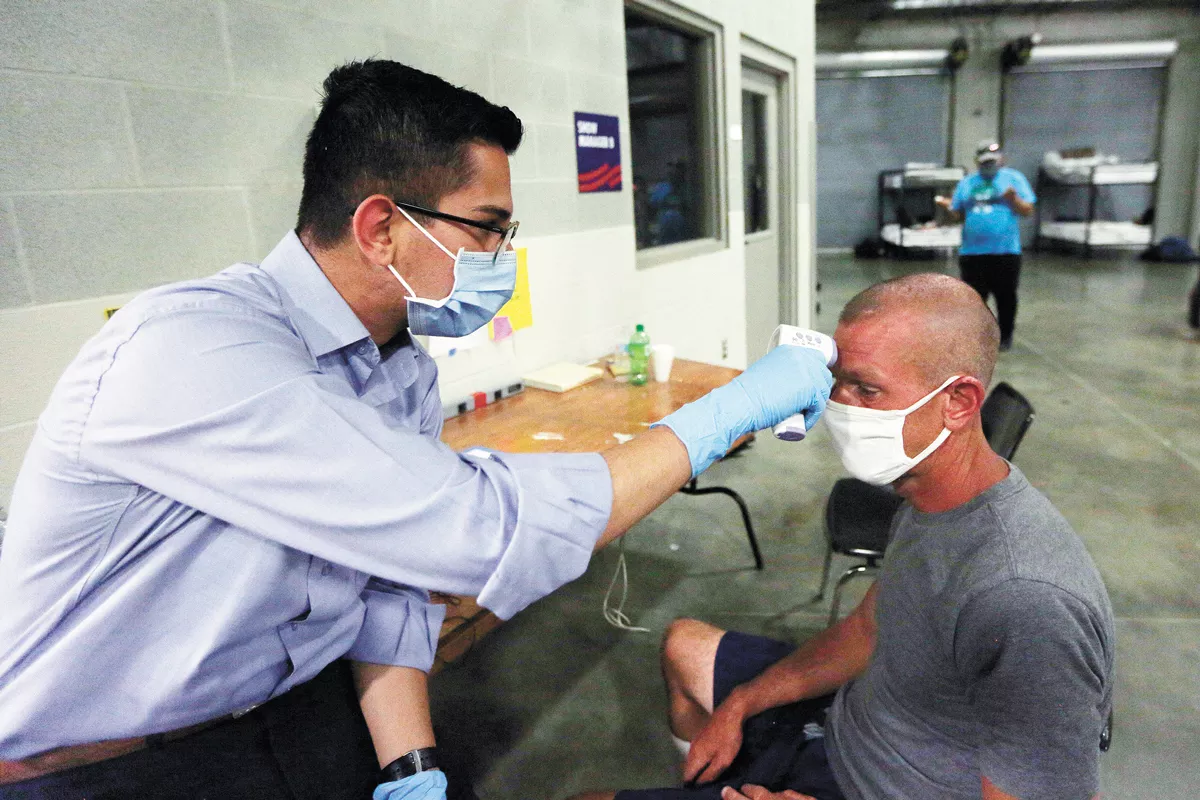
This year has been one like none other in any of our memories. The COVID-19 pandemic has thrust public health out in front, a seemingly strange place given it is typically behind the scenes. Spokane's first touch of the pandemic occurred when four cruise ship passengers, without symptoms, were cared for in Providence-Sacred Heart Medical Center's Special Pathogen Unit in February. The Spokane Regional Health District (SRHD)-Sacred Heart partnership demonstrated the importance of these two approaches to ensure the health of the community: prevention and clinical care. The effectiveness of safety protocols to prevent the spread of the infection to health care personnel, combined with the care they provided to their patients, was a foreshadowing of what we would experience in the months to come.
The emphasis on prevention, a foundational principle of public health, plays out regularly in our new daily routines. Non-pharmaceutical interventions, such as physical distancing, enhanced hand hygiene, and staying home when ill, were implemented during the pandemic of 1918 and have since been underlying practices to decrease the spread of a contagion. An important addition to these has been face masks, readily used in health care as "source control" to prevent the inadvertent spread of the infection by the wearer. (Would anyone want their surgeon to not wear a mask?) A prosocial behavior, as it benefits other community members, facial coverings are likely to also benefit the wearer by decreasing the volume of respiratory droplets they are exposed to. Commonplace in Asian countries following past epidemics, and quickly adopted by European countries as the COVID-19 pandemic spread across the continent, their benefits have been questioned in the U.S. This skepticism contributed to infection spread, especially by those either unaware of their developing infection or without symptoms, the latter possibly accounting for 40 percent of cases, according to the most recent COVID-19 Pandemic Planning Scenario provided by the Centers for Disease Control and Prevention (CDC).
Another core principle of public health is the importance of research and data to assist with making decisions that have population-level impact. The "novel coronavirus" has demonstrated advances in scientific knowledge and understanding do not follow a linear path. Rather, science progresses in fits and starts, sometimes leaps (of faith), paradigm shifts, followed by further questioning and then maybe an answer(s) that may not last the test of time. Think masks, hydroxychloroquine, respiratory droplet versus aerosol transmission, ventilators and intubation versus proning, and antiviral medications. In a New York Times opinion piece, Ashish Jha, dean of Brown University's School of Public Health, estimated that people infected today are roughly 30-50 percent less likely to die of the virus than they would have been in March or April, demonstrating how the science of medicine has evolved... and science matters.
Harm reduction, another public health fundamental, acknowledges the inherent risks of many activities or behaviors. We ask ourselves how best to minimize the risk knowing people will be people (think of seat belts, bike helmets and life vests). For COVID-19, the only way to eliminate all risk is to remain in self-isolation, which worked early during the Stay Home, Stay Healthy order, but is no longer feasible. Decreasing risk of infection is a balancing act of weighing options — outdoors is less risky than indoors, mask-wearing is safer than not, mask-wearing by everyone is the least risky, small groups are safer than large, interacting with others while staying more than 6 feet apart is less risky than being closer, and limited time spent with others is safer. While these inconveniences are just that, the risk of developing COVID-19 is a function of behaviors. You can pick and choose to practice a few or all, but the virus doesn't discriminate — it looks for opportunities.
As we have progressed through the COVID-19 pandemic, the challenges affecting us as individuals and as a community have been many. They have been perceived as a burden and infringement by some but were essential for all. Unfortunately, many will need to be continued, despite quarantine fatigue and wanting to "get back to normal." The virus didn't go away during the summer as had been predicted by some. Quite to the contrary, Spokane has seen 90 percent of its cases occur since the start of summer, most significantly after Memorial Day and Fourth of July. Consistent with past holidays, we're seeing an increase once again as summer closed with the three-day Labor Day weekend. The virus doesn't care about science-based metrics, but it does care about behaviors and readily takes advantage when evidence-based guidance is forgotten or willfully ignored. As we enter the fall, we will be driven indoors by colder weather, and the holidays will further challenge us as we seek togetherness, abandoning physical distancing. The COVID-19 virus will readily do what it does best — spread among those of us who have let down our guard.
Recently, Dr. Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota, compared COVID-19 to a wildfire, "We weren't sure what this coronavirus would do because we've never witnessed a pandemic of a coronavirus before. Now we know it's kind of a super forest fire. It just keeps burning and burning and burning wherever there is human wood." This reminded me of the Smokey the Bear advertisement, "Only you can prevent forest fires." Only you can prevent COVID-19. ♦
Dr. Bob Lutz is Spokane County's health officer. Opinions expressed are solely his.