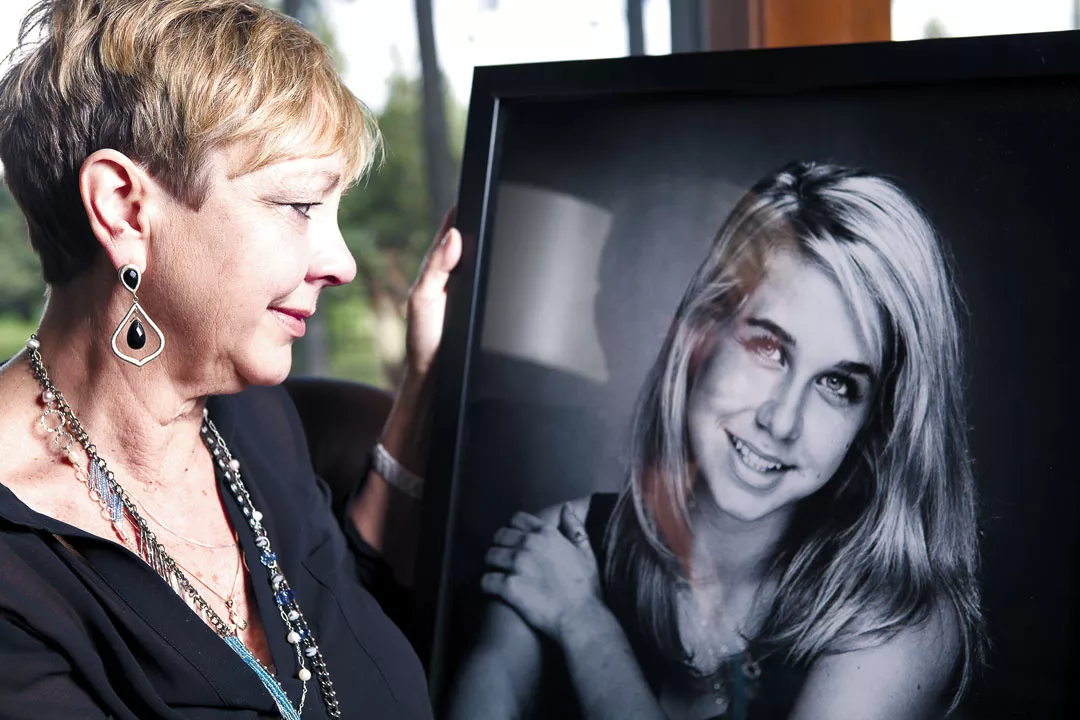
Debbie Hieber doesn’t go far without her best friend, Mary Lou Bonanzino. The stylish, 50-something girlfriends serve on nonprofit boards and drink coffee and wine together, depending on the time of day. They have more than once been shushed as they gossiped and laughed loudly in an otherwise quiet café.
Hieber especially needs her friend when she talks about her oldest daughter’s death, as she is doing today in a rather loud coffee shop.
Alyson, she begins to explain, died in September 2009. After struggling with bulimia all through high school and the start of college, her depleted 22-year-old body gave out.
Hieber suspects it started when Aly was a freshman in high school.
“She was throwing up. … She was taking laxatives, diuretics.” Hieber had tried to get Aly in Shadows to see local eating disorder specialists, but they were full.
“Aly went to general practitioners for help. They would tell her random things — ‘Don’t throw up anymore,’ ‘Watch your diet,’ ‘Come back in six months.’ I remember her saying, ‘I feel like there’s a demon inside me,’” says Hieber.
As Hieber recounts details of Aly’s last month of life, still grappling with unanswerable questions around it, her raw grief bubbles over. It’s hard to talk over the tears and loud din of less grave conversations going on around her. Her best friend steps in to provide details.
“When Aly first passed away, Debbie knew she was going to have to do something,” Bonanzino says. “As part of Debbie’s healing process and to bring meaning to a senseless tragedy, we’re trying to help INCED.”
Started by a group of local health care providers, the Inland Northwest Coalition on Eating Disorders has grown into an educational nonprofit group made up of therapists, dietitians and doctors with specialties in disordered eating. Through training and fundraising, members of INCED are expanding the awareness of, and conversations about, the lonely struggles with anorexia, bulimia and binge eating.
LOCAL HELP WANTED
“Ultimately, we want a full-scale treatment center,” says Bonanzino. She and the other members of INCED estimate that will cost a minimum of $1 million to start. “Now we’re offering a few workshops, in addition to fundraising efforts. I’d say we’re at the awareness stage,” she says.
“Other cities have this type of treatment,” says Hieber. The closest, the Moore Center in Bel supports INCED’s vision, even helping sponsor events in Spokane. But limited openings mean patients who need intensive treatment often must travel to other states.
Aly went to Arizona, where, Hieber recalls, she “was seeing a therapist, a nutritionist and an M.D. on a daily basis. When we were having the exit interview and they told us, ‘No one was available in Spokane’ [for the recommended fulltime monitoring following rehab], I told them I could find somebody. My sister had a friend here whose daughter was bulimic and had been seeing a therapist in Spokane. The friend was sure I could get Aly in.”
Hieber called the therapist but she had moved to Seattle. The counselors she knew about were booked. If a mother’s love and fierce determination were enough, Aly may have lived. But years of a binging and purging cycle and medication abuse had damaged her internal systems too much. She lived only 10 days past her discharge from rehab.
A HIDDEN DISEASE
“Rarely, if ever, do we see ‘eating disorder’ as a cause of death,” explains Krista Crotty, a psychologist who specializes in eating disorders. “It is more typically ‘heart failure,’ or other major organ or body-function failure that was likely caused from the eating disorder.”
Aly’s death certificate states “heart failure.”
“By the time she passed away, her teeth had rotted,” Debbie says quietly. “I remember thinking, ‘We’ll have to get her new teeth and, wait, maybe we should wait until she’s done throwing up.’ You worry about things you can see.”
It’s hard to characterize the intense anxiety people with eating disorders have around food, explains Crotty, who estimates that about 90 percent of her clients suffer from eating disorders. And because they are receiving treatment, they are among the fortunate. Estimates are that only one in 10 people with eating disorders gets help (some place that figure at one in 20). Still, 80 percent of those who manage to access care can’t get the intense treatment they need.
“Take the most terrifying thought you can: intentionally putting your children in danger, or jumping out this window with a bungee cord. That’s how people these people feel about food,” Crotty says. “A recovering alcoholic can stop going to bars, and a drug addict can stop meeting with his dealer, but we have to eat to survive.
“Most of the time we don’t celebrate without food, we don’t mourn without food,” Crotty adds. “We center meetings around meal times and coffee dates. The more we focus on food, the harder it is for an individual with an eating disorder to be able to talk openly about their fear and anxiety about food… They carry a lot of shame. There’s a part of them that wants help, but the eating disorder will tell you, ‘You’re useless and a failure’ if you can’t keep from eating. It’s this terrible mental collision.”
HEALING ISN’T EASY
Ponrat Pakpreo specializes in adolescent medicine and is one of few doctors in the community who seeks out patients with eating disorders. She offers training to doctors through her work with INCED.
“Some primary care doctors are comfortable managing eating disorders, some are not,” she admits. “I treat at all stages, from the prevention stage, when a young person has some self-esteem and dieting concerns, to inpatient management of medical complications from eating disorders, like persistent unhealthy eating or exercising, co-morbid mood issues and thoughts of suicide.”
Pakpreo says the first line of defense needs to be primary care providers. “Many patients have not disclosed concerns about body image or weight issues or even unhealthy eating behaviors to their providers, even though it has been going on for a long time. [Eating disorders] take a lot of time and patience and require providers to work closely with other team members, like therapists and dietitians.”
A local treatment center would be welcomed by the health care community, says Pakreo.
“It is especially helpful for adolescents whose parents either have to take a leave from work to be with their child or be separated from their children in treatment for extended periods of time.”
Hieber knows it will take a lot of fundraisers and a whole new set of conversations to bring the savagely secret burden of eating disorders out into the open.
“I want, so badly, for people to feel as comfortable discussing their eating disorder as they are in talking about the common cold, without the fear of being judged harshly by society,” says Hieber. “My goal right now is to not have anyone else go through this.”
To learn more, visit incedspokane.org.













