Thousands of times every day, doctors around the world look for issues inside their patients without ever breaking the skin, thanks to help from imaging technology like computed tomography (CT) scans, magnetic resonance imaging (MRI), X-ray and ultrasound.
But those machines can be expensive, running from hundreds to thousands of dollars per scan, depending on the technology, and in the case of CT scans and X-rays, they expose patients to varying degrees of radiation. While the scans often prevent unnecessary exploratory surgery and help physicians diagnose everything from cancer to strokes, the costs and radiation can be concerning, especially for patients who need frequent scans.
The good news is it looks like math can help.
That's right: math. Really, really complicated math — the kind that happens to be Melody Alsaker's passion.
Alsaker, an assistant professor of mathematics at Gonzaga University, is working with a team based at Colorado State University to improve a different kind of scan called electrical impedance tomography, or EIT.
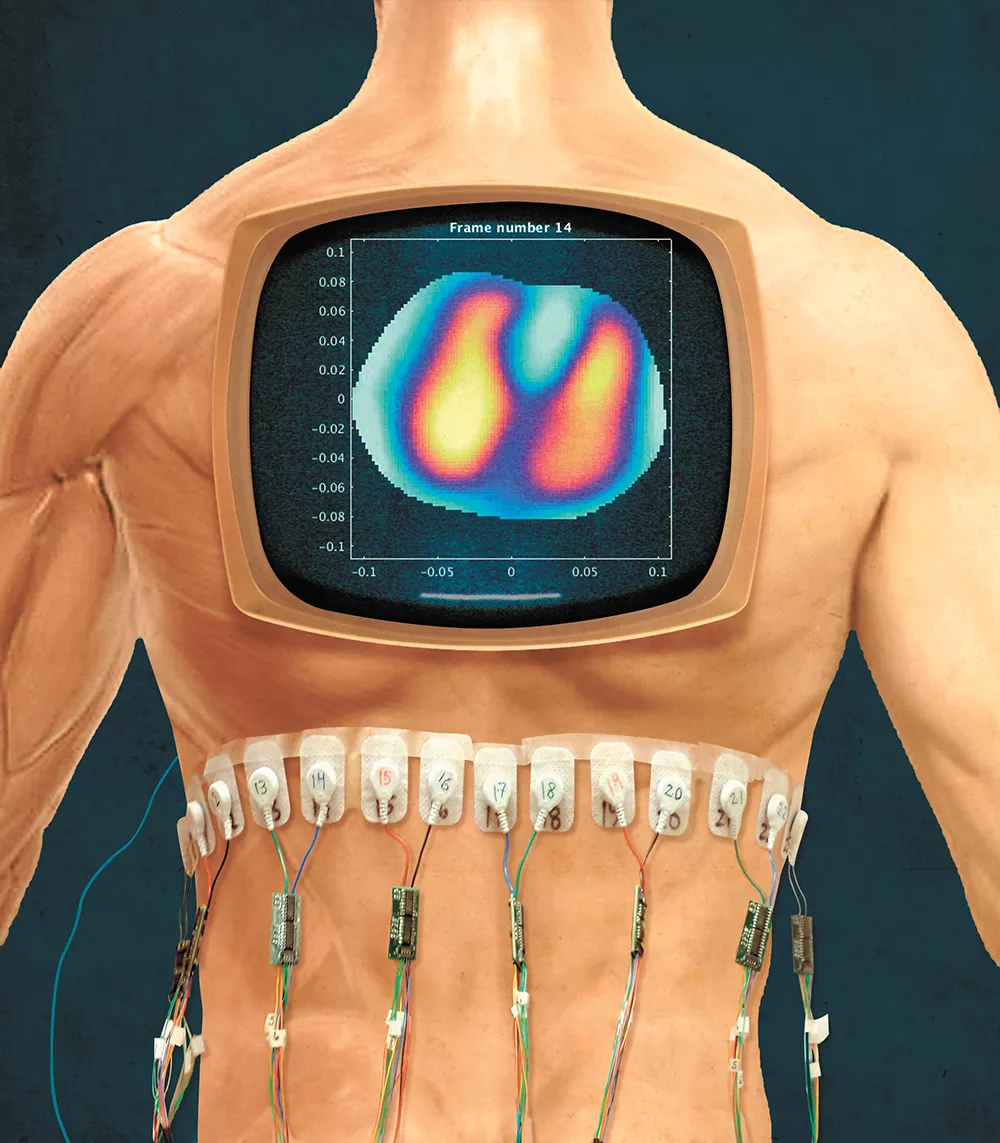
With EIT, electrodes are stuck around a patient in a circle to test electrical conductivity in that part of the body. Then a computer deciphers that data using mathematical algorithms to make a picture. Blood, for example, is really conductive, Alsaker says, while the air in your lungs isn't.
A major perk of EIT is that there isn't any ionizing radiation, she says, and the machine is much cheaper and easier to move around."The machine is very portable," Alsaker says. "You can wheel it in on a cart. You could put it in an ambulance, you can put it in a helicopter, you can take it to the patient's bedside. Or for patients who are immobile, like a car crash victim, or in war zones, or in places without good medical facilities, you can take the machine to people."
Alsaker worked in the EIT lab at Colorado State while earning her Ph.D. and essentially wrote the computer code that turns the data into pictures.
Due to the way the data is crunched to make images that show a slice of the body, it's difficult to get the pictures to the same resolution offered by other scans, Alsaker says.That's partly because electricity travels in three dimensions and the EIT machine is trying to make a two-dimensional image, she says, and partly because the math question they're using to convert the images doesn't have a very stable solution: very small differences or "noise" in the data can make for big errors.
"Some of these other technologies like MRI and CT and so forth, which have their advantages and drawbacks, they're just mathematically easier processes," Alsaker says. "That's a big part of why EIT is an active area of research for mathematicians and engineers, because there's still a lot of technical difficulties that need to be worked out."
A major part of her work now is centered on figuring out how to filter out that noise in the data without losing definition, so it's easier to see the edges of organs and tissues."I'm actively trying to figure out how to clean up the spatial resolution," Alsaker says. "Because of the difficulties of the math problem involved, it's been a little bit slow to get this to where it's a usable technology, despite the advantages."
Potential applications for EIT are being tested all the time.
The group Alsaker is working with out of Colorado has partnered with a children's hospital there to test whether EIT scans could replace some tests done on children with cystic fibrosis, a rare genetic disorder that affects the lungs.
"Cystic fibrosis patients get regions of air entrapment in their lungs, and they often come in yearly for CT scans," Alsaker says. "If you can replace some of the CT scans with these EIT scans, it's better for them."
The technology could also be used in place of another test that's used to measure lung volume, she says, making it possible to get accurate measurements on small children and patients who can't follow directions or aren't physically able to sit up.
EIT also does a good job of collecting a lot of images in a short time frame, which enables researchers to compile the images and basically make a movie, she says. For example, you could show a patient breathing.
"You can see, in real time, the air entering and exiting the lungs," Alsaker says. "This is being studied for use on patients on ventilators, because you can actually injure patients by having improper settings."
While it may take time to continue improving the technology, Alsaker remains hopeful for its ability to help in the future.
"There are a lot of problems to solve still. It's a hard math problem," she says. "But, if we could get this working in hospitals and so forth, it does have a lot of potential." ♦